State Laws on School Nursing Outline Copious Responsibilities for Nurses
As students returned to school in fall 2021, school nurses played a critical role in ensuring the ongoing health and safety of students. Though school nurses have historically led efforts to mitigate the spread of communicable diseases, their role has shifted significantly over time, and new COVID-19 responsibilities only added to school nurses’ already full plates. Even before the pandemic, school nurses were responsible for a wide range of tasks, including managing chronic disease, creating and coordinating individual student health plans, administering and storing medications, training school staff in emergency procedures and medication administration, and keeping and reporting records and health information. School nurses typically performed these services for multiple school buildings (as of 2017, only 39.3 percent of schools had a full time school nurse). Now, school nurses have become responsible for administering COVID-19 tests; helping with vaccination clinics; facilitating immunizations and health screenings that had been disrupted during remote learning; conducting contact tracing; enforcing general COVID protocols; and providing COVID-19 education to students, staff, and families—all in addition to their regular duties.
State statutes and regulations dictate not only whether schools are required to employ a school nurse, but also what qualifications they must have and what they must do once they arrive in school buildings. Moreover, state policies highlight whether and how the role of a school nurse is valued, particularly as an expert in the wake of public health crises like COVID-19. Understanding the current landscape of state statutes and regulations that govern school nursing is critical to identifying opportunities to better support and elevate school nurses’ role as longstanding pillars of public health.
Child Trends, in partnership with EMT Associates, analyzed the landscape of state statutes and regulations as of October 2021 to better understand how such policies define the role of school nurses (see Methodology). This brief presents our findings.
Findings
State policies on whether districts must employ school nurses
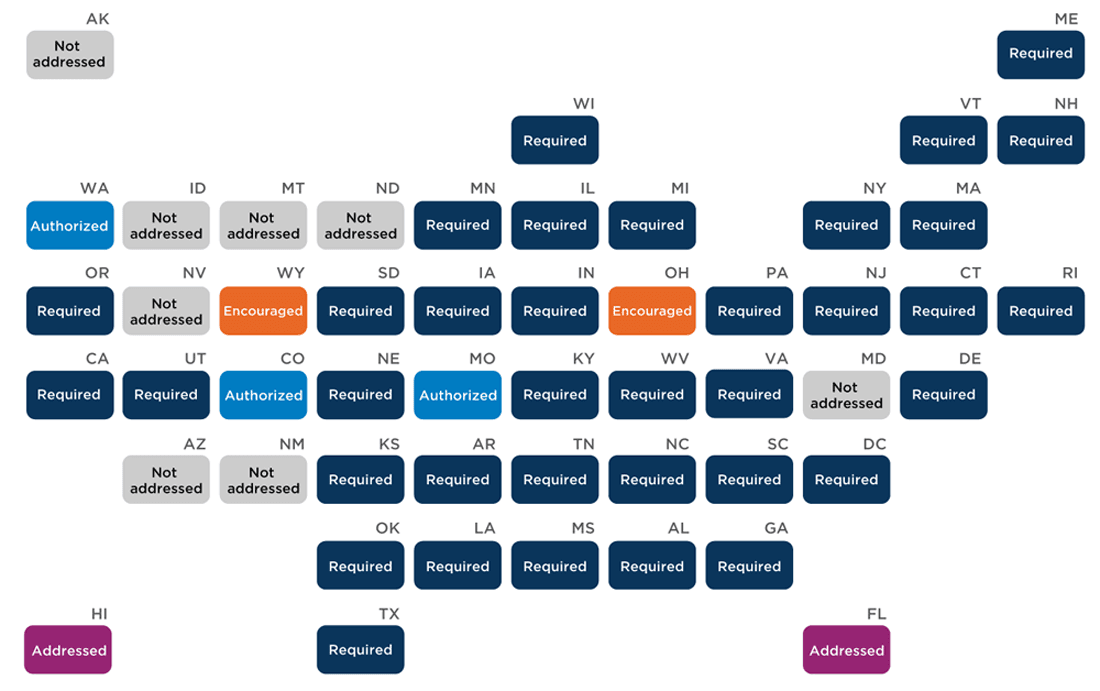
Thirty-five states and the District of Columbia (DC) have policies requiring (“must,” “shall”) the employment of school nurses, while another seven states authorize (“may”), encourage (“should”), or address making school nurses available to students (Appendix A). However, even among states that require making school nurses available, those requirements range from full-time nurses in each school to part-time nurses providing services to several schools to nurses employed at the LEA level. For example, two states (Delaware and Vermont) require full-time nurses in every school, and an additional twelve states (Alabama, Arkansas, Georgia, Indiana, Iowa, Oregon, Pennsylvania, Tennessee, Utah, Vermont, Virginia, and West Virginia) set recommended or required nurse-to-student ratios, though these ratios go unheeded by many districts. Notably, those ratios range from 1:500 (Alabama, Vermont) to 1:3,000 (Tennessee), while the Centers for Disease Control and Prevention recommends a ratio of one school nurse for every 750 students. Eight states (Alaska, Arizona, Idaho, Maryland, Montana, Nevada, New Mexico, and North Dakota) do not address requirements for school districts to employ school nurses.
State policies on whether districts must employ school nurses
State policies on school nurses’ qualifications
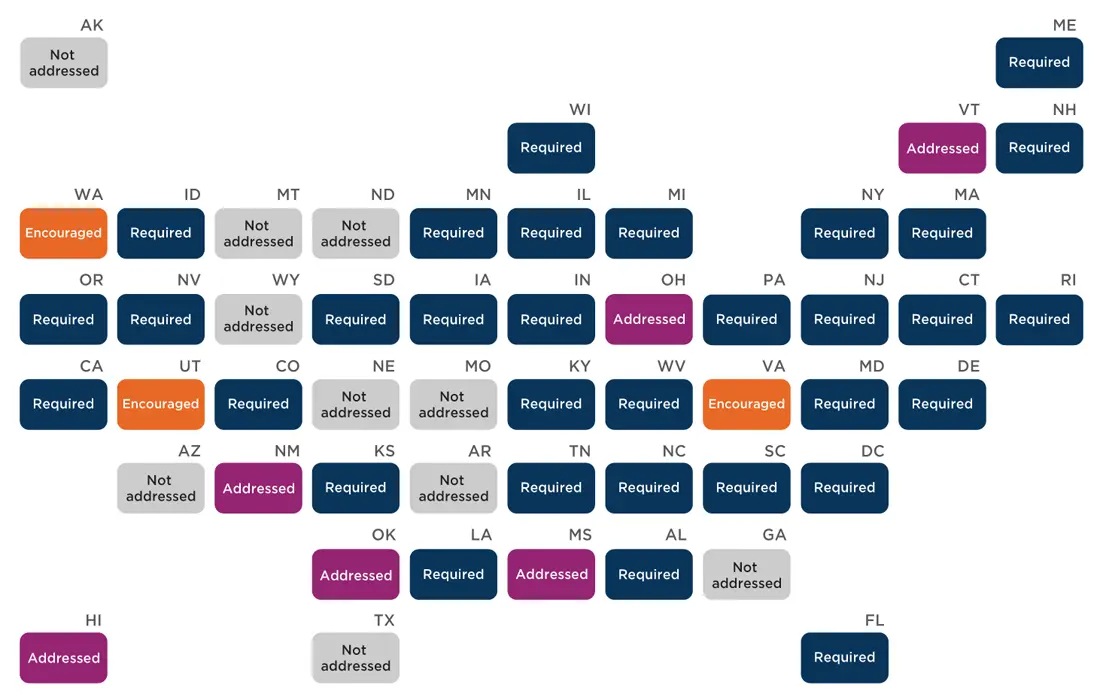
Thirty-one states and DC have policies that require specific educational qualifications or licenses/certifications for school nurses, while another nine states discuss licensing, certification, and educational qualifications by encouraging (discussing the benefits of) or addressing (by defining) such qualifications (Appendix B). Most states require school nurses to be licensed as a registered nurse (RN) by the state board of nursing with a bachelor’s or master’s degree from an accredited institution. Other permitted licenses and certifications for school nurses include licensed practical nurses (LPNs) (Alabama, Mississippi, New Hampshire, South Carolina), licensed public health nurses (Washington, Wisconsin), certified nursing assistants (CNAs) (New Hampshire), and certified nurse practitioners (CNPs) (Tennessee). Fourteen states’ departments of education (California, Connecticut, Delaware, Illinois, Indiana, Michigan, Nevada, New Hampshire, New Jersey, New Mexico, Ohio, Oregon, Vermont, West Virginia) require additional educational course work to receive and then maintain a state certification as a school nurse, in addition to the RN state license. Other common qualifications for school nurses include certification in first aid, cardiopulmonary resuscitation (CPR), and automatic external defibrillator (AED) use.
Some states’ policies authorize non-certified staff to provide supplemental services, such as medication administration, emergency care, or health screenings, if they are trained and supervised by a registered school nurse.
State policies on school nurses’ qualifications
State policies on school nurses’ role in managing chronic conditions
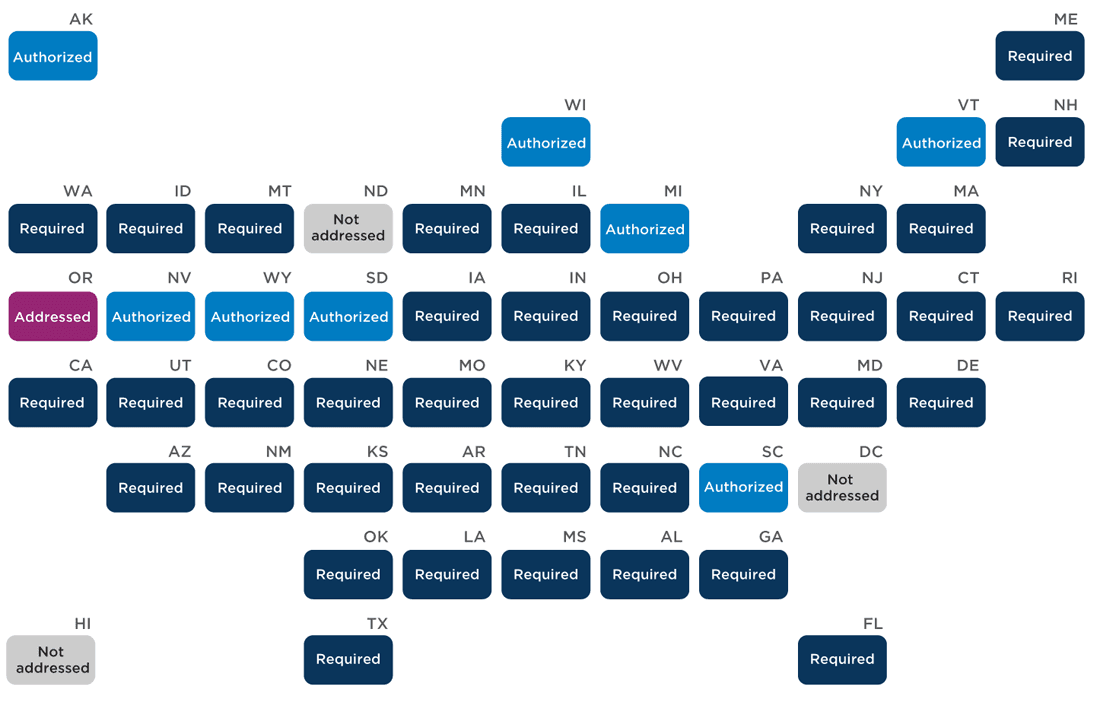
Forty-eight states have policies that describe school nurses’ role in managing chronic conditions, including allergies, diabetes, and seizures (Appendix C). Responsibilities include storing and administering medication; developing and implementing student health plans related to these conditions; and training other school personnel on chronic disease care (e.g., recognizing symptoms, emergency administration of medication). Of these, 39 states require (“must,” “shall”) a registered (or otherwise properly licensed or certified) nurse to perform these services, while eight states authorize (“may”) but do not require school nurses to fill these roles, giving some flexibility to who performs these duties. Oregon addresses the non-liability of school nurses, school administrators, teachers, or other school staff related to administering medication or supervising student self-administration of medication. Notably, there is a nationwide school nurse shortage, which may mean that schools are asking staff without proper medical training to perform these duties, even when the state requires proper licensure or certification. Schools may put students at risk when non-nurses perform duties that should be performed by qualified individuals.
State policies on school nurses’ role in managing chronic conditions
State policies on school nurses’ role in administering medication
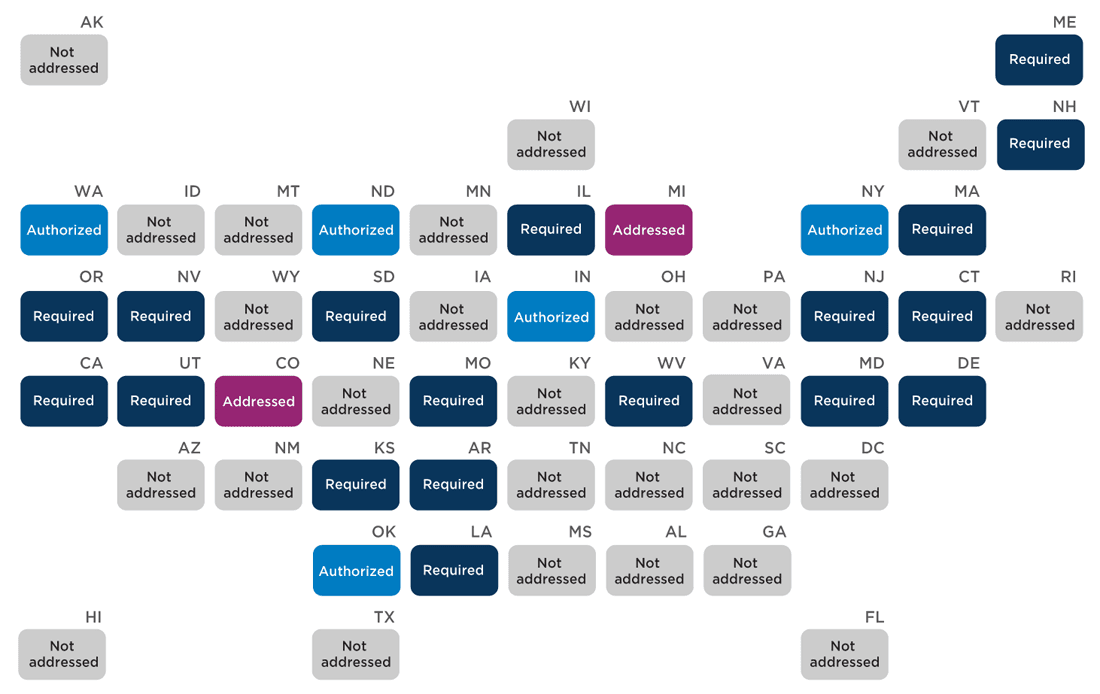
Twenty-five states have policies that describe school nurses’ role in administering medication beyond what is specifically required for managing chronic conditions (Appendix D). These responsibilities include storing and administering students’ prescription medicine, managing students’ health records and parental consents, training other school personnel to administer prescription medication as permitted by parents or guardians, and assessing students’ ability to self-administer medication. Of states with policies addressing medication administration, 18 specifically require (“must,” “shall”) school nurses to perform these duties, while five states authorize (“may”) but do not require school nurses to fill these roles, which allows unlicensed assistive personnel, school administrators, teachers, or other school staff to perform these duties.
State policies on school nurses’ role in administering medication
State policies on school nurses’ role in developing and managing student health plans
Twenty-one states have policies that describe school nurses’ role in developing and managing student health plans for chronic conditions such as allergies, asthma, diabetes, and seizures as well as other individualized health care needs (Appendix E). Responsibilities addressed include training other school personnel and volunteer health aides on proper procedures of care; collaborating with students, parents or guardians, and primary care physicians; developing protocol for emergency response; and storing emergency stock medication. Of the states that govern school nurses’ role in student health plans, 17 require (“must,” “shall”) a registered nurse to be involved in creating individualized student health and emergency action plans, while two states authorize (“may”) but do not require school nurses to assist students who require individualized health care services. Importantly, the assessment and care planning can be done only by an RN—assessment is not in the scope of practice for LPNs. In cases where an RN is not present, student care plans may not exist or are provided from outside healthcare providers, often without proper adaption to the school setting or school-specific needs.
State policies on school nurses’ role in developing and managing student health plans
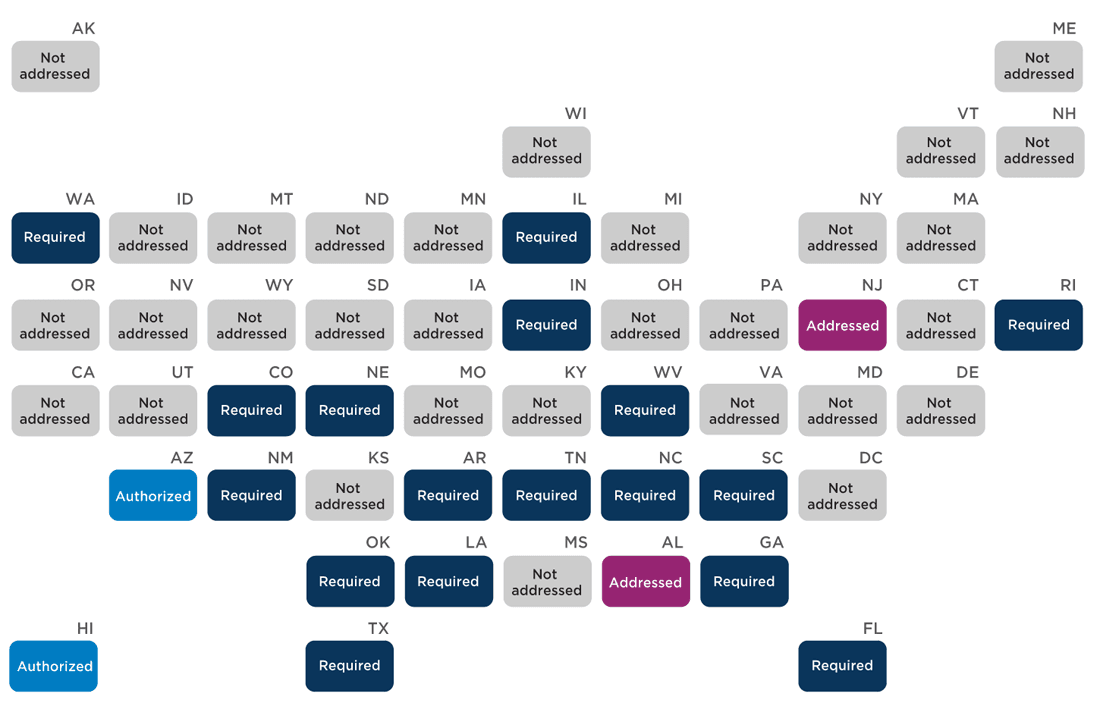
State policies on school nurses’ role in student health screenings
Twenty-five states have policies that describe school nurses’ roles in health screenings—including vision, hearing, dental, BMI, scoliosis, dyslexia, lead exposure, and general physical health (Appendix F). Their responsibilities range from scheduling, facilitating, documenting results, and/or referring students for follow-up care. Nineteen states require (“must,” “shall”) school nurses to conduct or oversee these screenings, receive training on specific screenings or examinations, or train other personnel to conduct the screenings, while six states authorize (“may”) or encourage (“recommend,” “should”) but do not require school nurses to fill these roles.
State policies on school nurses’ role in student health screenings
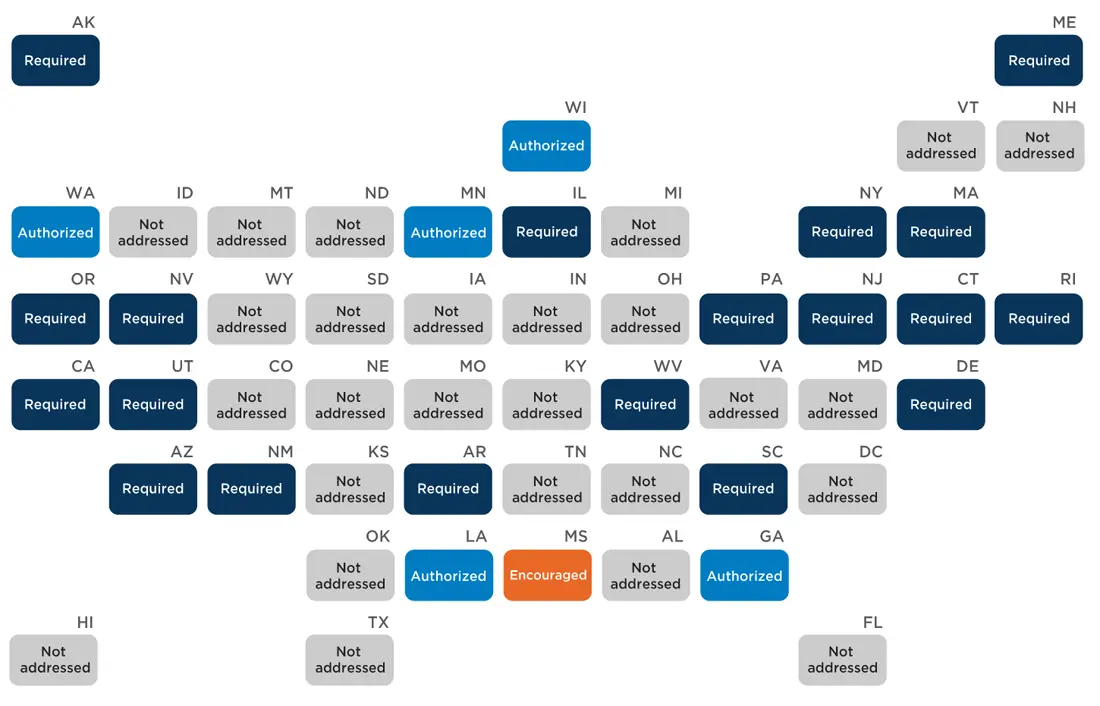
State policies on school nurses’ role in student immunizations
Twelve states have policies that describe school nurses’ role in facilitating and/or keeping records of student immunizations (Appendix G). Of these, ten states detail requirements for school nurses to administer immunizations, facilitate immunization programs or clinics, or keep or access records of student immunizations. New Mexico authorizes school nurses to access the immunization registry, while Texas authorizes school nurses to submit a written statement of a student’s immunity or disease history in lieu of a vaccine record for varicella.
State policies on school nurses’ role in student immunizations
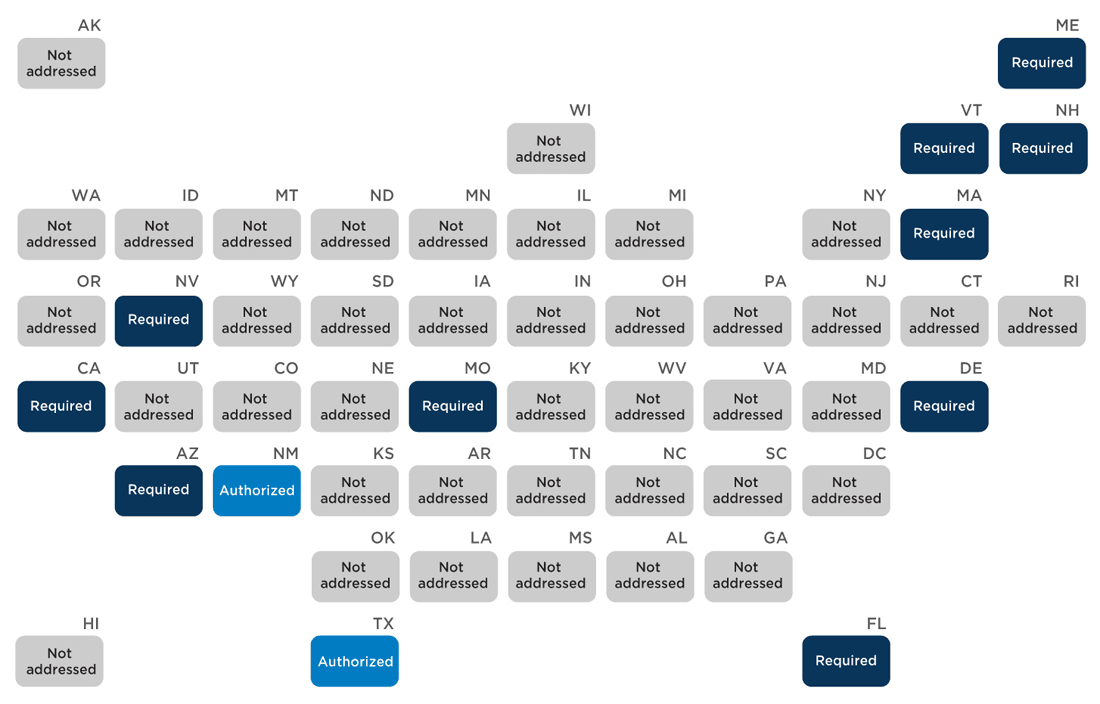
State policies on school nurses’ role in infectious disease control
Eighteen states and DC have policies that describe school nurses’ role in mitigating the spread of contagious diseases (Appendix H). Of these, five states (Maine, New York, Oregon, Pennsylvania, West Virginia) and DC require schools to exclude students from school who have been exposed to a communicable disease or who are showing signs of illness as reported to them by school nurses, while four states (Massachusetts, New Jersey, Oklahoma, Wisconsin) authorize but do not require schools to do so. Oregon and Pennsylvania’s policies require nurses to determine when excluded students are no longer communicable and may be readmitted, while Idaho, Oklahoma, and New York authorize but do not require school nurses to perform this duty. Three states (Georgia, Maine, Pennsylvania) and DC require school personnel to consult with the school nurse when a student is suspected of having a communicable disease, while nine states (Idaho, Iowa, Maryland, Massachusetts, Nebraska, New Mexico, Oregon, West Virginia, Wisconsin) and DC require school nurses to report suspected cases of communicable diseases to state and local public health agencies.
State policies on school nurses’ role in infectious disease control
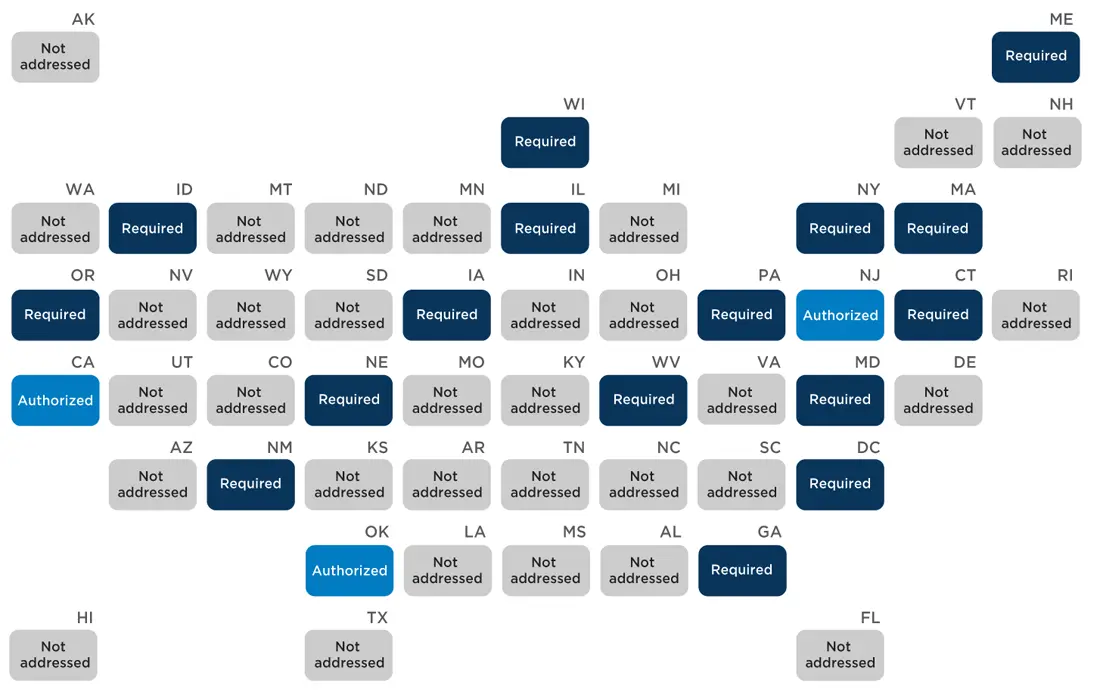
State policies on school nurses’ role in COVID-19
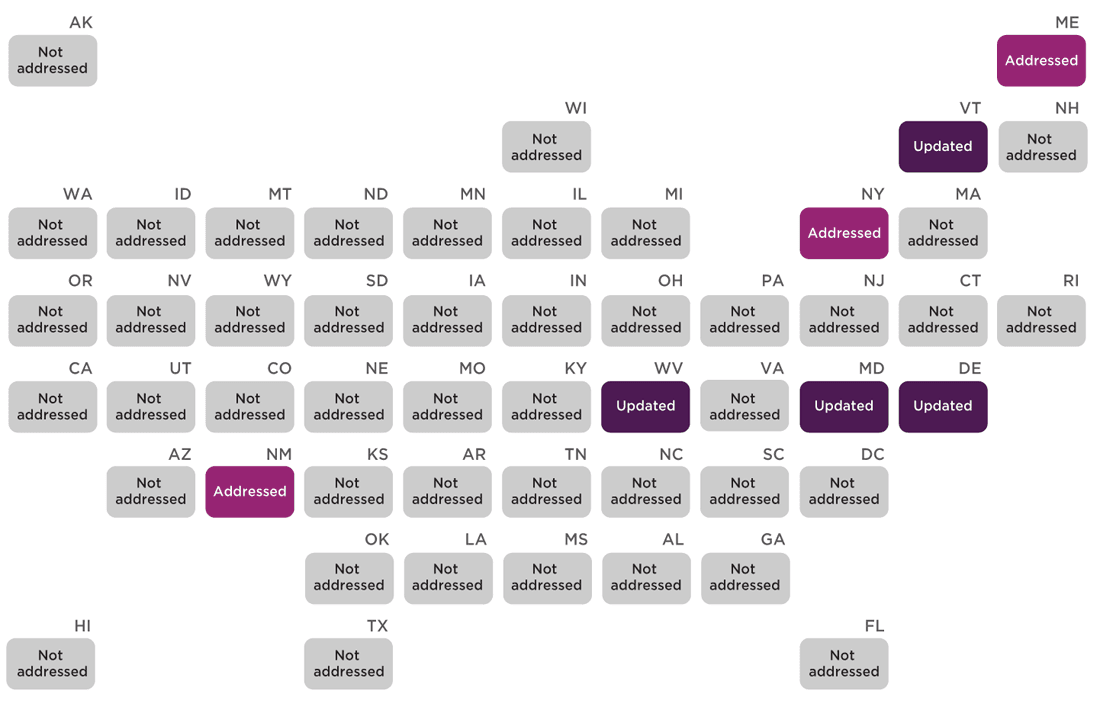
As of October 2021, policies in three states explicitly addressed school nurses’ role in COVID-19. New Mexico requires school nurses to use the Centers for Disease Control and Prevention (CDC) recommended transmission-based precautions when caring for sick people. New York allowed health examinations, including hearing, vision, and scoliosis screenings to be waived during the 2020-2021 school year due to COVID-19. Maine also updated an existing regulation on comprehensive health and safety and emergency management plans to require involving school nurses, physicians, and public health staff in developing and annually updating those plans. Four additional states (Delaware, Maryland, Vermont, and West Virginia) updated policies referencing either immunization or communicable disease between March 2020 and October 2021; however, these policies do not specifically mention COVID-19. Delaware also passed emergency legislation on COVID-19 Mitigation and Prevention requiring mask use by all students, faculty, staff, and visitors inside school buildings; however, the policy does not delegate a person responsible for ensuring that the policy is implemented or enforced.
State policies on school nurses’ role in COVID-19
Discussion and Conclusion
Our analysis examined how states govern the roles, responsibilities, and requirements for school nurses through policy. These policies often determine the availability of nurses in school buildings, the daily responsibilities they perform in service to their students, and expectations for how they will contribute to public health. The COVID-19 pandemic added significantly to existing responsibilities as school nurses stepped in to administer COVID-19 tests; conduct contact tracing; educate staff, students, and families on COVID-19 precautions, such as proper mask wearing, hand washing and hygiene, and physical distancing; update school-based health protocols and safety plans; and support decision making for school closing/reopening plans. The pandemic has increased the need for school nurses—who address and support efforts related to chronic absenteeism and the impact of health conditions on academic outcomes—and added to school nurses’ direct care responsibilities as students return to school demonstrating worsened physical and mental health.
Our analysis was necessarily limited: although we examined the landscape of state policies, we did not evaluate their effect in practice. The presence or absence of state-level policy pertaining to school nurses does not preclude the existence of non-codified guidance, nor does it indicate whether or how well policies are being implemented. However, from what is codified, we can assess the baseline expectations of school nurses. School nurses are required to fulfill numerous codified responsibilities around coordinating care or providing direct health services in all 50 states and DC and have been asked to take on even more during the COVID-19 pandemic. Despite these copious and ever-increasing demands, few states have policies that set a strong floor for school nurse capacity in schools—just twelve states have policies addressing recommended or required nurse-to-student ratios and only two require a full-time nurse in every school. By establishing policies that improve school nurses’ capacity, states can vest power in nurses’ deep expertise to lead their school communities’ health and wellness efforts on behalf of students and staff.
Methodology
To analyze the current landscape of state statutes and regulations related to school nursing practice, Child Trends and EMT Associates identified codified policies using a series of keyword Boolean searches in LexisNexis and Westlaw that reference school nursing. Policies repealed before October 2021 were not included in the search, nor were policies passed after this date or pending legislative action. Based on the content of each identified policy, researchers at EMT Associates conducted memoing to describe unique categories of policies. They then coded each identified policy based on its degree of prescriptiveness (addressed, encouraged, authorized, or required). Our analysis focused on the following research questions:
- How do states govern the availability of school nurses?
- How do states govern certifications or qualifications for school nurses?
- What are school nurses authorized to do?
- What are school nurses required to do?
- How are school nurses engaged in public health efforts?
- What specific responsibilities do school nurses have with respect to the COVID-19 pandemic?
Suggested Citation
Steed, H., O’Toole, D., Lao, K., Nuñez, B., Surani, K., & Stuart-Cassel, V. (2022). State laws on school nursing outline copious responsibilities for nurses. Child Trends. https://doi.org/10.56417/2161j1674h
This publication is supported by cooperative agreement NU87PS004367-01-01 funded by the Centers for Disease Control and Prevention (CDC). Its contents are solely the responsibility of the authors and do not necessarily represent the official views or endorsement of the CDC or the Department of Health and Human Services.
Appendices
Appendix A - Availability
Appendix B - Certification
Appendix C - Services - Chronic
Appendix D - Services - MA
Appendix E - Services - SHP
Appendix F - Services - Screenings
Appendix G - Immunization
Appendix H - Communicable
Appendix I - COVID
© Copyright 2024 ChildTrendsPrivacy Statement
Newsletter SignupLinkedInThreadsYouTube